What Are The 4 Stages Of Rheumatoid Arthritis? At WHAT.EDU.VN, we understand the importance of recognizing these stages for effective management and early intervention. Our goal is to provide clear and accessible information about the progression of rheumatoid arthritis, empowering you to take proactive steps towards your health and well-being. We are here to help you navigate every step of your healthcare journey, offering support and guidance. Explore rheumatoid arthritis progression, disease advancement, and joint degeneration with us today.
Table of Contents
- Understanding Rheumatoid Arthritis (RA)
- 1.1. What is Rheumatoid Arthritis?
- 1.2. Why Knowing the Stages Matters
- The First Steps: Early Rheumatoid Arthritis
- 2.1. Stage 1: Very Early RA
- 2.1.1. Common Signs
- 2.1.2. How It’s Diagnosed
- 2.2. Stage 2: Mild Rheumatoid Arthritis
- 2.2.1. Common Signs
- 2.2.2. How It’s Diagnosed
- 2.1. Stage 1: Very Early RA
- As RA Progresses: Later Stages
- 3.1. Stage 3: Moderate Rheumatoid Arthritis
- 3.1.1. Common Signs
- 3.1.2. How It’s Diagnosed
- 3.2. Stage 4: Severe Rheumatoid Arthritis
- 3.2.1. Common Signs
- 3.2.2. How It’s Diagnosed
- 3.1. Stage 3: Moderate Rheumatoid Arthritis
- Treating RA at Each Stage
- 4.1. Starting Early
- 4.2. Treating Moderate RA
- 4.3. Managing Severe RA
- Frequently Asked Questions
- 5.1. How is RA different from osteoarthritis?
- 5.2. Can osteoarthritis turn into RA?
- 5.3. Can X-rays show the difference?
- Need Help?
1. Understanding Rheumatoid Arthritis (RA)
1.1. What is Rheumatoid Arthritis?
Rheumatoid arthritis is a chronic autoimmune disease that primarily affects the joints, causing inflammation and damage. Unlike osteoarthritis, which results from wear and tear on the joints, rheumatoid arthritis is an autoimmune disorder. This means that the body’s immune system mistakenly attacks its own tissues, specifically the synovium, the lining of the joints. According to the Mayo Clinic, rheumatoid arthritis can affect other organs, including the skin, eyes, lungs, heart, and blood vessels.
1.2. Why Knowing the Stages Matters
Understanding the different stages of RA is very important for effective disease management. By knowing the stage, patients and doctors can make better decisions about treatment, lifestyle changes, and overall care. Early detection and treatment can significantly slow disease progression and improve quality of life. Recognizing the specific symptoms and challenges associated with each stage allows for a more tailored and effective approach to care. Remember, at WHAT.EDU.VN, we are dedicated to offering the most current and practical information to help you in your healthcare journey.
2. The First Steps: Early Rheumatoid Arthritis
2.1. Stage 1: Very Early RA
In the very early stages of rheumatoid arthritis, symptoms can be mild and easily overlooked. Stage 1 is marked by inflammation of the joint lining, leading to pain, stiffness, and swelling. Catching RA at this stage is crucial because early treatment can significantly alter the course of the disease.
2.1.1. Common Signs
- Mild joint pain: This is often the first sign, and it may come and go.
- Slight joint swelling: You might notice that some joints, especially in your hands and feet, appear puffy.
- Stiffness: Joints may feel stiff, especially in the morning or after periods of inactivity.
- Fatigue: Some people experience a general feeling of tiredness.
2.1.2. How It’s Diagnosed
Diagnosing RA in Stage 1 can be difficult, as symptoms are not always clear. Doctors typically use a combination of:
- Physical exam: Checking for joint swelling, tenderness, and range of motion.
- Blood tests: Looking for markers like rheumatoid factor (RF) and anti-citrullinated protein antibodies (ACPA), as well as inflammatory markers like C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR).
- Imaging tests: X-rays, ultrasounds, or MRIs can help detect early joint damage.
2.2. Stage 2: Mild Rheumatoid Arthritis
In Stage 2, the inflammation in the joints begins to cause damage to cartilage, the protective tissue that cushions the joints. Patients may experience increased pain and stiffness, and the range of motion in the affected joints may be limited.
2.2.1. Common Signs
- Persistent joint pain: The pain becomes more constant and noticeable.
- More pronounced swelling: Joint swelling becomes more evident and affects daily activities.
- Morning stiffness: Stiffness lasts longer, often for several hours in the morning.
- Decreased range of motion: Difficulty moving joints fully.
2.2.2. How It’s Diagnosed
Diagnosis in Stage 2 usually involves:
- Physical exam: Assessing the extent of joint damage and inflammation.
- Blood tests: Monitoring levels of RF, ACPA, CRP, and ESR to track disease activity.
- Imaging tests: X-rays and MRIs to assess cartilage and bone damage.
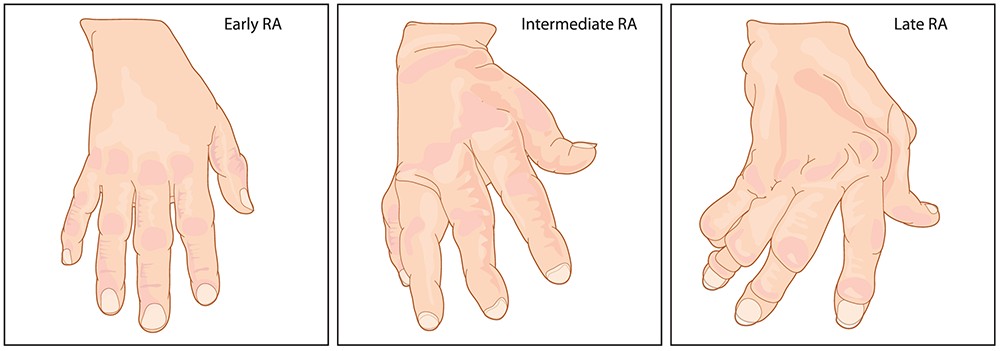 Rheumatoid arthritis in the hands showing swelling and joint deformity The image depicts hands affected by rheumatoid arthritis, illustrating swelling and joint deformity as the disease progresses, leading to visible changes in the hands and fingers.
Rheumatoid arthritis in the hands showing swelling and joint deformity The image depicts hands affected by rheumatoid arthritis, illustrating swelling and joint deformity as the disease progresses, leading to visible changes in the hands and fingers.
3. As RA Progresses: Later Stages
3.1. Stage 3: Moderate Rheumatoid Arthritis
In Stage 3, the disease progresses to a moderate level. The inflammation continues to damage the cartilage and bone within the joints. This stage is often marked by increased pain, swelling, and decreased range of motion. Patients may also experience fatigue and the formation of rheumatoid nodules, which are firm lumps that develop under the skin around affected joints.
3.1.1. Common Signs
- Severe pain in the affected joints: The pain becomes more intense and persistent.
- Visible rheumatoid nodules: These nodules can appear near the elbow, hands, or other affected areas.
- Carpal tunnel syndrome: Inflammation around the wrist can lead to nerve compression, causing numbness and tingling in the hand.
- Evidence of joint damage in imaging studies: X-rays and MRIs show clear signs of cartilage and bone damage.
3.1.2. How It’s Diagnosed
Diagnosing RA at Stage 3 involves:
- Physical exam: Assessing joint function, range of motion, and the presence of rheumatoid nodules.
- Blood tests: Monitoring elevated levels of inflammatory markers.
- Imaging tests: X-rays, MRIs, and ultrasounds to evaluate the extent of joint damage.
3.2. Stage 4: Severe Rheumatoid Arthritis
Stage 4 is the most severe stage of rheumatoid arthritis. At this point, there is significant joint damage and deformity, which can lead to severe pain, decreased mobility, and reduced quality of life. The joints may become unstable, and patients may experience chronic fatigue and a general feeling of being unwell.
3.2.1. Common Signs
- Extreme joint pain and swelling: The pain is often constant and debilitating.
- Significant joint deformity: Joints may become visibly deformed.
- Decreased range of motion to the point of disability: Patients may have difficulty performing daily activities.
- Chronic fatigue and a pervasive feeling of being unwell: The systemic effects of RA become more pronounced.
3.2.2. How It’s Diagnosed
Diagnosis at Stage 4 typically involves:
- Physical exam: Assessing the extent of joint damage and functional limitations.
- Blood tests: Showing consistently high levels of inflammatory markers.
- Imaging tests: X-rays and MRIs revealing extensive joint damage and bone erosion.
4. Treating RA at Each Stage
4.1. Starting Early
Early intervention is key to managing rheumatoid arthritis effectively. Treatment typically includes:
- Nonsteroidal anti-inflammatory drugs (NSAIDs): To reduce pain and inflammation.
- Disease-modifying antirheumatic drugs (DMARDs): To slow down disease progression and prevent further joint damage. Common DMARDs include methotrexate, sulfasalazine, and hydroxychloroquine.
- Corticosteroids: To reduce inflammation and pain, often used as a short-term treatment option.
4.2. Treating Moderate RA
Treatment for moderate RA may involve a combination of:
- DMARDs: Continued use of DMARDs to control inflammation and slow disease progression.
- Biologic agents: These medications target specific parts of the immune system to reduce inflammation. Examples include TNF inhibitors (such as etanercept and infliximab) and non-TNF biologics (such as abatacept and rituximab).
- Physical therapy: To maintain joint function and improve range of motion.
- Occupational therapy: To help patients adapt to daily activities and protect their joints.
4.3. Managing Severe RA
Managing severe RA requires a comprehensive approach:
- Aggressive medications: Biologic DMARDs and other advanced therapies to control inflammation and prevent further joint damage.
- Pain management: Medications and therapies to manage chronic pain.
- Surgical interventions: Joint replacement surgery may be necessary to relieve pain and improve function.
- Supportive care: Including physical therapy, occupational therapy, and counseling to help patients cope with the physical and emotional challenges of RA.
Remember, understanding rheumatoid arthritis is a continuous journey. At WHAT.EDU.VN, we are committed to providing the resources and support you need.
5. Frequently Asked Questions
5.1. How is RA different from osteoarthritis?
Osteoarthritis (OA) and rheumatoid arthritis (RA) are both forms of arthritis, but they have different causes and characteristics. OA is caused by the breakdown of cartilage in the joints due to wear and tear, while RA is an autoimmune disease where the body’s immune system attacks the joints. According to the Arthritis Foundation, OA typically develops slowly over time and primarily affects weight-bearing joints, such as the knees, hips, and spine. RA, on the other hand, can affect any joint in the body and often causes systemic symptoms like fatigue and fever.
5.2. Can osteoarthritis turn into RA?
No, osteoarthritis cannot turn into rheumatoid arthritis. They are distinct conditions with different underlying causes. However, it is possible for a person to have both OA and RA at the same time. Having both conditions can complicate diagnosis and treatment, so it’s important to work with a healthcare provider who is knowledgeable about both types of arthritis.
5.3. Can X-rays show the difference?
Yes, X-rays can help differentiate between osteoarthritis and rheumatoid arthritis. In OA, X-rays may show joint space narrowing, bone spurs, and other signs of cartilage breakdown. In RA, X-rays may reveal joint erosion, swelling, and inflammation. According to the American College of Rheumatology, imaging tests like X-rays and MRIs are important tools for diagnosing and monitoring arthritis.
6. Need Help?
Do you have more questions about rheumatoid arthritis or other health concerns? At WHAT.EDU.VN, we’re here to provide you with the answers you need. Don’t hesitate to ask any question, no matter how big or small. Our team of experts is dedicated to providing reliable, easy-to-understand information to help you make informed decisions about your health. Contact us today and let us help you navigate your healthcare journey.
Address: 888 Question City Plaza, Seattle, WA 98101, United States
Whatsapp: +1 (206) 555-7890
Website: WHAT.EDU.VN
Don’t struggle with unanswered questions. Visit what.edu.vn now and ask away! Your health matters, and we’re here to help.