Mouth ulcers, also known as canker sores, are a common and often painful condition that affects many people. These small sores develop on the soft tissues inside your mouth, such as the cheeks, lips, tongue, and gums. While most mouth ulcers are harmless and heal on their own within a couple of weeks, understanding what causes them can help you manage and potentially prevent them. This article delves into the various factors that contribute to the development of mouth ulcers, providing a comprehensive guide to their causes, symptoms, and available treatments.
What Are Mouth Ulcers?
A mouth ulcer is essentially an erosion or break in the mucous membrane, the delicate lining inside your mouth. Medically termed as mucosal lesions or oral ulcers, they disrupt the smooth, healthy tissue, exposing the sensitive layers underneath. These lesions can vary in size and severity, but they are typically characterized by a whitish or yellowish center surrounded by a red, inflamed border.
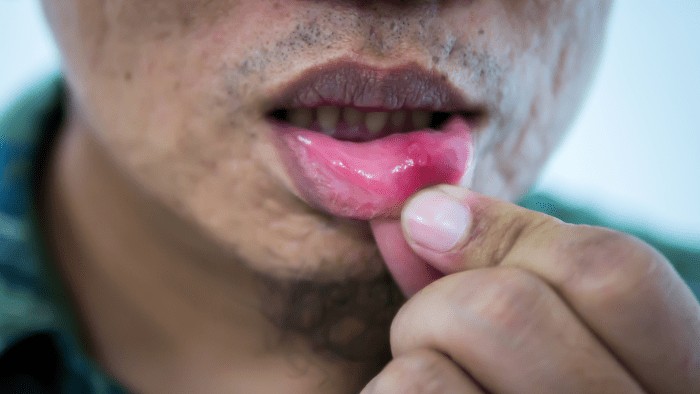 Visible mouth ulcer inside lower lip, a common symptom of oral health issues.
Visible mouth ulcer inside lower lip, a common symptom of oral health issues.
Common Causes of Mouth Ulcers
The reasons behind mouth ulcers are diverse, ranging from simple injuries to underlying health conditions. Here’s a breakdown of the most frequent culprits:
1. Injury or Trauma
Physical injury is one of the most common triggers for mouth ulcers. This can occur due to:
- Accidental cheek biting: An unintentional bite to the inside of your cheek or lip is a frequent cause.
- Toothbrush injury: Slipping while brushing your teeth can lead to abrasions and ulcers.
- Sharp teeth or dental appliances: Misaligned, broken, or sharp teeth, as well as poorly fitting dentures, braces, or retainers, can constantly rub against the oral tissues, causing irritation and ulcers.
- Burns: Consuming hot foods or liquids can burn the delicate mucous membrane, leading to ulcer formation.
2. Aphthous Ulcers (Canker Sores)
Aphthous ulcers, commonly known as canker sores, are recurrent mouth ulcers that affect a significant portion of the population. While the exact cause remains unknown for most individuals, several factors are believed to play a role:
- Idiopathic nature: In many cases, aphthous ulcers appear without a clear identifiable trigger.
- Nutritional deficiencies: In a subset of people, deficiencies in essential nutrients like Vitamin B12, folate, or iron have been linked to recurrent aphthous ulcers. Addressing these deficiencies may help reduce their occurrence.
Aphthous ulcers typically appear on the softer linings of the mouth, such as the inner lips and cheeks, the underside of the tongue, the floor of the mouth, the soft palate, and around the tonsils. They are usually small, often less than 5mm in diameter, but multiple ulcers can occur simultaneously and sometimes merge. These ulcers generally heal within 10 to 14 days, but they are known for their tendency to recur at varying intervals.
3. Infections
Various infections can manifest as mouth ulcers:
- Viral infections: The herpes simplex virus, responsible for cold sores, can also cause ulcers inside the mouth, especially during primary infections. Other viral infections can also contribute.
- Bacterial and fungal infections: While less common, bacterial and fungal infections can also lead to oral ulcers, particularly in individuals with weakened immune systems.
4. Medications and Irritants
Certain substances can irritate the oral mucosa and lead to ulceration:
- Medications: Some medications can have side effects that include mouth ulcers.
- Strong antiseptics: Overuse or undiluted strong mouthwashes can irritate the delicate tissues, causing ulcers.
5. Skin Conditions
Certain skin conditions can also affect the mouth and cause ulcers:
- Lichen planus: This inflammatory condition can manifest in the mouth as lacy white patches, red swollen tissues, and open sores.
6. Autoimmune Diseases
Autoimmune diseases, where the body’s immune system mistakenly attacks its own tissues, can sometimes cause mouth ulcers.
7. Nutritional Deficiencies
As mentioned earlier, deficiencies in certain vitamins and minerals can contribute to mouth ulcers, particularly aphthous ulcers. These include Vitamin B12, folate, and iron.
8. Gastrointestinal Diseases
Certain gastrointestinal conditions are associated with an increased risk of mouth ulcers:
- Crohn’s disease and Celiac disease: These inflammatory bowel diseases are sometimes linked to oral ulcers.
9. Medical Conditions and Stress
Overall health and stress levels can also play a role:
- Underlying medical conditions: Certain systemic illnesses can increase susceptibility to mouth ulcers.
- Stress, illness, and fatigue: Periods of stress, illness, or extreme tiredness can sometimes worsen or trigger mouth ulcers.
10. Mouth Cancer
Although less frequent, a persistent mouth ulcer that doesn’t heal can be a sign of mouth cancer. It is crucial to be aware of this possibility, especially if you have risk factors like tobacco and alcohol use.
Symptoms of Mouth Ulcers
The symptoms of mouth ulcers can vary depending on the cause, but common indicators include:
- Painful sores: One or more painful sores on the mucous membrane lining of the mouth are the hallmark symptom.
- Inflammation: The mucous membrane around the sores may appear swollen and red.
- Chewing and brushing difficulties: Tenderness can make chewing and tooth brushing uncomfortable.
- Irritation from food: Spicy, salty, or sour foods can exacerbate the pain.
- Denture or appliance discomfort: Dentures, orthodontic aligners, or mouth splints can irritate the sores.
- Painless ulcers (rare): In some serious cases, like mouth cancer, ulcers may surprisingly be painless.
When to Seek Medical Advice
While most mouth ulcers resolve on their own, it’s important to seek professional advice in certain situations:
- Ulcers lasting over 2 weeks: If a mouth ulcer persists for more than two weeks without healing, consult a dentist or doctor.
- Frequent recurrence: If you experience mouth ulcers frequently, it’s worth investigating potential underlying causes.
- Ulcers interfering with daily life: If ulcers are making it difficult to eat, drink, or speak, seek medical help.
- Suspicion of underlying conditions: If you suspect a nutritional deficiency, gastrointestinal issue, or any other underlying medical condition, consult your doctor.
- Concerns about mouth cancer: Especially if you use tobacco or alcohol regularly, do not ignore a non-healing ulcer.
Treatment Options for Mouth Ulcers
For most common mouth ulcers, treatment focuses on managing symptoms and preventing complications, as they typically heal naturally.
- Avoid irritants: Steer clear of spicy, salty, and sour foods that can aggravate ulcers.
- Stay hydrated: Drink plenty of fluids to keep the mouth moist.
- Maintain oral hygiene: Gently brush your teeth to keep the mouth clean and prevent secondary infections.
- Antiseptic gels: Over-the-counter antiseptic gels can be applied to ulcers to promote healing and reduce pain.
- Salt water rinse: Rinsing your mouth with warm, slightly salted water several times a day can help soothe ulcers and keep them clean.
- Medicated mouthwash: Alcohol-free medicated mouthwashes, preferably containing chlorhexidine gluconate, can be used twice daily to reduce bacteria.
- Topical steroids: In some cases, dentists or specialists may prescribe topical steroid mouthwashes or ointments to reduce inflammation.
- Immunosuppressants (severe cases): For severe or persistent ulcers, particularly those related to autoimmune conditions, immunosuppressant medications might be prescribed by a healthcare professional.
Prevention of Mouth Ulcers
While not always preventable, you can reduce your risk of mouth ulcers by:
- Gentle brushing: Use a soft toothbrush and brush gently to avoid trauma to the gums and inner cheeks.
- Balanced diet: Eating a nutritious diet rich in vitamins and minerals can help prevent deficiency-related ulcers.
- Manage underlying conditions: If you have underlying medical conditions, ensure they are well-managed to reduce the risk of secondary mouth ulcers.
Conclusion
Mouth ulcers are a common annoyance, often caused by minor injuries or aphthous ulcers. While usually harmless and self-healing, understanding the diverse range of potential causes—from infections and medications to nutritional deficiencies and underlying medical conditions—is crucial for effective management and prevention. Pay attention to the duration and frequency of your mouth ulcers, and don’t hesitate to seek medical advice if you have concerns, especially regarding non-healing ulcers or potential underlying health issues.