What Is Anc? It’s a vital blood test measurement! WHAT.EDU.VN provides clear explanations and helps you understand its significance. Seeking clarity on medical terms and their impact on health? Explore reliable health information and get your questions answered on WHAT.EDU.VN, covering complete blood count and neutrophil levels with educational resources.
1. Defining Absolute Neutrophil Count (ANC)
The absolute neutrophil count, often shortened to ANC, is a critical measure of neutrophils in your blood. But what is ANC, specifically? To understand, let’s break it down. Neutrophils are a type of white blood cell (WBC) essential for fighting off infections, particularly bacterial infections. They are part of the immune system. The ANC indicates the total number of these infection-fighting cells present in your body. This measurement helps healthcare professionals assess your immune system’s ability to combat infections.
A healthy ANC range typically falls between 2,500 and 6,000 neutrophils per microliter of blood. When the ANC is within this range, it suggests that your body has an adequate supply of neutrophils to defend against most infections. However, deviations from this range can signal potential health concerns. An ANC below 1,000 neutrophils per microliter is termed neutropenia, indicating a higher risk of infection. Severely low ANC levels, such as those below 500, significantly increase the risk of life-threatening infections.
1.1 The Role of White Blood Cells
To fully grasp the significance of ANC, it’s essential to understand the role of white blood cells (WBCs). WBCs are the body’s defense force, protecting against infections, foreign invaders, and even cancerous cells. Different types of WBCs specialize in different aspects of immune defense. Neutrophils are the most abundant type of WBC and play a crucial role in the initial response to bacterial infections.
1.2 Neutrophils: The First Responders
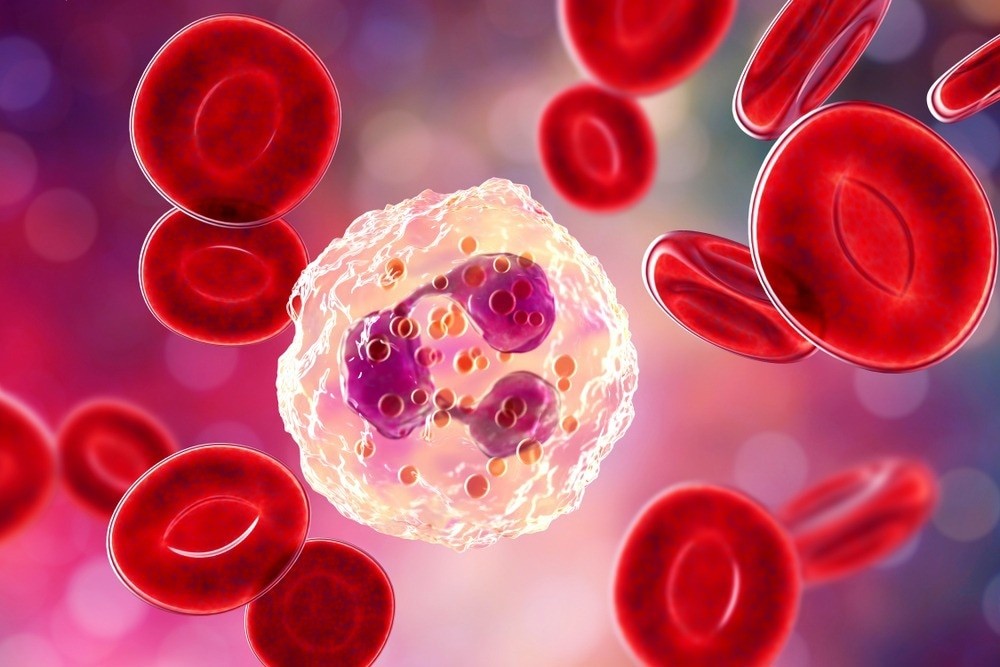
Neutrophils act as the first responders when the body detects a bacterial invasion. They quickly migrate to the site of infection and engulf the bacteria, effectively neutralizing the threat. They achieve this through a process called phagocytosis, where they surround and ingest the bacteria.
Image Credit: Microscopic view of neutrophil, a type of white blood cell.
1.3 Polys and Bands: Different Stages of Neutrophils
Neutrophils exist in different stages of maturity in the blood:
- Polys (Segmented Neutrophils): These are mature neutrophils, fully capable of fighting infections. They are the most abundant type of neutrophil in a healthy individual.
- Bands (Stab Cells): These are immature neutrophils. An elevated number of bands can indicate that the bone marrow is working hard to produce more neutrophils, often in response to an infection.
Understanding the roles of polys and bands provides a more complete picture of the body’s immune response.
2. ANC Calculation: How is ANC Determined?
Calculating the ANC involves a simple formula, but it requires understanding the components derived from a complete blood count (CBC). The CBC provides information about the different types of cells in your blood, including WBCs and the percentage of each type of WBC.
2.1 The ANC Formula
The ANC is calculated using the following formula:
ANC = Total WBC count x (Percentage of Neutrophils / 100)
Here, percentage of neutrophils is the sum of percentage of segmented neutrophils (polys) and percentage of band neutrophils.
2.2 Example Calculation
Let’s illustrate this with an example:
Suppose a person has a WBC count of 5,000 per microliter.
The differential count shows that neutrophils (polys) make up 50% of the WBCs, and bands make up 5%.
- Add the percentages of polys and bands: 50% + 5% = 55%
- Convert the percentage to a decimal: 55% / 100 = 0.55
- Multiply the total WBC count by the decimal: 5,000 x 0.55 = 2,750
Therefore, the ANC in this case is 2,750 neutrophils per microliter, which falls within the normal range.
2.3 Interpreting the Results
Once you have the ANC, it’s crucial to interpret the results correctly. Here’s a quick guide:
- Normal ANC (2,500 – 6,000/µL): Indicates a healthy immune system with an adequate supply of neutrophils.
- Mild Neutropenia (1,000 – 1,500/µL): Slightly increased risk of infection.
- Moderate Neutropenia (500 – 1,000/µL): Moderate risk of infection. Precautions may be necessary.
- Severe Neutropenia (Below 500/µL): High risk of severe and life-threatening infections. Immediate medical attention is required.
2.4 Factors Affecting ANC
Several factors can influence ANC levels, including:
- Infections: Infections can temporarily increase ANC as the body produces more neutrophils to fight the infection.
- Medications: Certain medications, such as chemotherapy drugs, can lower ANC.
- Underlying Medical Conditions: Conditions like leukemia or autoimmune disorders can affect neutrophil production and ANC levels.
Understanding these factors is important for accurately interpreting ANC results.
3. Neutropenia: What Does Low ANC Mean?
Neutropenia, defined as an ANC below 1,000 neutrophils per microliter, indicates a deficiency of neutrophils in the blood. This condition compromises the body’s ability to fight off infections, making individuals more susceptible to bacterial, fungal, and viral infections. The severity of neutropenia is classified based on the ANC level:
- Mild Neutropenia: 1,000 – 1,500 neutrophils/µL
- Moderate Neutropenia: 500 – 1,000 neutrophils/µL
- Severe Neutropenia: Below 500 neutrophils/µL
The lower the ANC, the higher the risk of infection.
3.1 Causes of Neutropenia
Neutropenia can arise from various causes, including:
- Chemotherapy: Chemotherapy drugs often target rapidly dividing cells, including neutrophils, leading to a decrease in ANC.
- Bone Marrow Disorders: Conditions like leukemia or myelodysplastic syndromes can impair the bone marrow’s ability to produce neutrophils.
- Autoimmune Diseases: Autoimmune disorders, such as rheumatoid arthritis or lupus, can cause the body to attack and destroy neutrophils.
- Infections: Certain infections, like HIV, hepatitis, or Lyme disease, can lead to neutropenia.
- Medications: Besides chemotherapy, other medications, such as antibiotics or anticonvulsants, can sometimes cause neutropenia.
- Vitamin Deficiencies: Deficiencies in vitamins like B12 or folate can impair neutrophil production.
- Congenital Disorders: Some individuals are born with genetic conditions that affect neutrophil production, leading to chronic neutropenia.
3.2 Symptoms of Neutropenia
Often, neutropenia itself doesn’t cause specific symptoms. Instead, individuals with neutropenia are more likely to develop infections, which can manifest with various symptoms, including:
- Fever: A high fever is often the first sign of infection in individuals with neutropenia.
- Sore Throat: Infections can cause painful sore throats.
- Mouth Sores: Mouth ulcers or sores can develop due to infections.
- Pneumonia: Neutropenia increases the risk of pneumonia, leading to cough, chest pain, and difficulty breathing.
- Skin Infections: Skin infections can occur more easily, leading to redness, swelling, and pus formation.
- Diarrhea: Infections in the digestive system can cause diarrhea.
3.3 Diagnosis of Neutropenia
Neutropenia is typically diagnosed through a complete blood count (CBC). If the CBC reveals a low ANC, further tests may be necessary to determine the underlying cause. These tests can include:
- Bone Marrow Biopsy: This procedure involves taking a small sample of bone marrow to examine it under a microscope. It can help identify bone marrow disorders affecting neutrophil production.
- Blood Tests: Additional blood tests can help detect infections, autoimmune disorders, or vitamin deficiencies that may be contributing to neutropenia.
3.4 Management and Treatment of Neutropenia
The management of neutropenia depends on the underlying cause and the severity of the condition. Treatment strategies may include:
- Treating Underlying Infections: If neutropenia is caused by an infection, antibiotics, antifungals, or antiviral medications may be prescribed to eliminate the infection.
- Granulocyte Colony-Stimulating Factors (G-CSFs): G-CSFs are medications that stimulate the bone marrow to produce more neutrophils. They are commonly used to manage chemotherapy-induced neutropenia.
- Discontinuing Offending Medications: If a medication is suspected of causing neutropenia, it may be discontinued or replaced with an alternative.
- Dietary Changes: Addressing vitamin deficiencies through dietary changes or supplements can help improve neutrophil production.
- Protective Measures: Individuals with neutropenia are advised to take precautions to minimize their risk of infection, such as:
- Frequent handwashing
- Avoiding crowds and sick individuals
- Wearing a mask in public places
- Avoiding raw or undercooked foods
3.5 Complications of Neutropenia
The primary complication of neutropenia is an increased risk of infection. Infections can be severe and life-threatening, requiring prompt medical attention. Other potential complications include:
- Sepsis: A systemic inflammatory response to infection that can lead to organ damage and failure.
- Pneumonia: A lung infection that can cause severe respiratory distress.
- Invasive Fungal Infections: Infections caused by fungi that can spread throughout the body.
3.6 Neutropenic Diet
A neutropenic diet is often recommended for individuals with neutropenia to reduce the risk of foodborne infections. This diet involves avoiding certain foods that are more likely to harbor bacteria or other pathogens, such as:
- Raw or undercooked meats, poultry, and seafood
- Raw fruits and vegetables
- Unpasteurized dairy products
- Soft cheeses
It is essential to consult with a healthcare professional or registered dietitian to develop a personalized neutropenic diet plan.
Image Credit: Illustration depicting neutropenia, a medical condition characterized by low levels of neutrophils in the blood.
4. ANC and Cancer Treatment: Why is ANC Important in Cancer Patients?
ANC plays a crucial role in cancer treatment, particularly for patients undergoing chemotherapy. Chemotherapy drugs, while effective at killing cancer cells, can also damage healthy cells, including those in the bone marrow responsible for producing neutrophils. This can lead to chemotherapy-induced neutropenia, which significantly increases the risk of infection in cancer patients.
4.1 Monitoring ANC During Chemotherapy
Regular monitoring of ANC is essential during chemotherapy to assess the impact of treatment on the patient’s immune system. Frequent blood tests are performed to track ANC levels and detect neutropenia early.
4.2 Adjusting Chemotherapy Dosage
If a patient develops neutropenia during chemotherapy, the healthcare team may need to adjust the dosage of chemotherapy drugs or delay subsequent treatment sessions. This allows the bone marrow time to recover and produce more neutrophils.
4.3 Predicting Neutropenic Events
ANC levels can help predict the likelihood of neutropenic events, such as fever or infections, after chemotherapy. This allows healthcare professionals to proactively implement preventive measures.
4.4 Determining the Need for Antibiotics
ANC helps determine whether antibiotics or other measures are needed to prevent or treat infections in cancer patients with neutropenia. Prophylactic antibiotics may be prescribed to reduce the risk of bacterial infections.
4.5 Isolation Precautions
Inpatient cancer patients with low ANC may need to be isolated to protect them from exposure to infectious agents. Outpatient cancer patients with neutropenia are advised to avoid crowds and individuals with flu or colds.
4.6 Granulocyte Colony-Stimulating Factors (G-CSFs) in Cancer Treatment
G-CSFs are commonly used in cancer treatment to stimulate the bone marrow to produce more neutrophils. These medications can help reduce the duration and severity of neutropenia, allowing patients to continue chemotherapy with fewer interruptions.
4.7 ANC as a Predictor of Outcomes
ANC can also serve as a predictor of treatment outcomes in cancer patients. Patients with higher ANC levels during chemotherapy tend to have better responses to treatment and improved survival rates.
5. Factors That Can Affect Your ANC
Several factors can influence your ANC levels, leading to either an increase or decrease in neutrophil count. Understanding these factors can help you better interpret your ANC results and take appropriate steps to manage your health.
5.1 Infections
Infections are a common cause of elevated ANC levels. When your body detects an infection, it responds by producing more neutrophils to fight the invading pathogens. This increase in neutrophil production can lead to neutrophilia, a condition characterized by an abnormally high ANC.
5.2 Medications
Certain medications can affect ANC levels, either increasing or decreasing neutrophil production. Chemotherapy drugs are well-known for causing neutropenia by damaging bone marrow cells responsible for producing neutrophils. Other medications that can cause neutropenia include:
- Antibiotics
- Anticonvulsants
- Antithyroid drugs
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
Medications that can increase ANC levels include:
- Corticosteroids
- Lithium
- Epinephrine
5.3 Medical Conditions
Underlying medical conditions can also affect ANC levels. Conditions that can cause neutropenia include:
- Leukemia
- Myelodysplastic syndromes
- Autoimmune disorders (e.g., rheumatoid arthritis, lupus)
- Vitamin deficiencies (e.g., B12, folate)
- Infections (e.g., HIV, hepatitis)
Conditions that can cause neutrophilia include:
- Inflammatory conditions (e.g., inflammatory bowel disease, vasculitis)
- Stress
- Surgery
- Trauma
- Certain cancers
5.4 Lifestyle Factors
Lifestyle factors, such as smoking and excessive alcohol consumption, can also influence ANC levels. Smoking can increase ANC levels, while excessive alcohol consumption can decrease ANC levels.
5.5 Age
ANC levels can vary with age. Newborns typically have higher ANC levels than adults. ANC levels tend to decline with age, particularly in older adults.
5.6 Ethnicity
Certain ethnic groups, such as African Americans, may have lower normal ANC ranges compared to other ethnic groups. This is known as benign ethnic neutropenia and is not typically associated with an increased risk of infection.
5.7 Pregnancy
ANC levels can change during pregnancy. Neutrophil counts tend to increase during pregnancy, particularly in the later stages.
5.8 Stress
Physical or emotional stress can temporarily increase ANC levels. This is because stress hormones, such as cortisol, can stimulate the release of neutrophils from the bone marrow into the bloodstream.
6. Maintaining a Healthy ANC: Tips and Recommendations
Maintaining a healthy ANC is essential for a robust immune system and overall well-being. While some factors affecting ANC are beyond your control, such as underlying medical conditions or certain medications, there are several lifestyle and dietary measures you can take to support a healthy neutrophil count.
6.1 Diet and Nutrition
A balanced and nutritious diet is crucial for supporting a healthy immune system and maintaining a normal ANC. Here are some dietary recommendations:
- Eat Plenty of Fruits and Vegetables: Fruits and vegetables are rich in vitamins, minerals, and antioxidants that boost immune function.
- Consume Adequate Protein: Protein is essential for building and repairing tissues, including immune cells.
- Include Healthy Fats: Healthy fats, such as omega-3 fatty acids, can help reduce inflammation and support immune function.
- Get Enough Vitamin B12 and Folate: Vitamin B12 and folate are essential for cell growth and division, including neutrophil production.
- Consider Probiotics: Probiotics can help maintain a healthy gut microbiome, which plays a crucial role in immune function.
- Avoid Processed Foods, Sugary Drinks, and Excessive Alcohol: These can impair immune function and negatively affect ANC levels.
6.2 Hygiene Practices
Good hygiene practices are essential for preventing infections, which can affect ANC levels. Here are some hygiene recommendations:
- Wash Your Hands Frequently: Wash your hands thoroughly with soap and water, especially after using the bathroom, before eating, and after being in public places.
- Practice Good Oral Hygiene: Brush your teeth regularly and see your dentist for checkups to prevent oral infections.
- Avoid Touching Your Face: Avoid touching your eyes, nose, and mouth to prevent the spread of germs.
- Keep Surfaces Clean: Regularly clean and disinfect frequently touched surfaces, such as doorknobs, countertops, and light switches.
6.3 Lifestyle Modifications
Certain lifestyle modifications can help support a healthy ANC:
- Quit Smoking: Smoking can impair immune function and increase the risk of infections.
- Limit Alcohol Consumption: Excessive alcohol consumption can suppress immune function and decrease ANC levels.
- Manage Stress: Chronic stress can weaken the immune system. Practice stress-reducing activities, such as yoga, meditation, or spending time in nature.
- Get Enough Sleep: Aim for 7-8 hours of sleep per night to support optimal immune function.
- Exercise Regularly: Regular physical activity can boost immune function and improve overall health.
6.4 Vaccinations
Staying up-to-date on vaccinations can help protect you from infections that can affect ANC levels. Talk to your doctor about recommended vaccinations based on your age, health status, and lifestyle.
6.5 Regular Medical Checkups
Regular medical checkups are essential for monitoring your ANC levels and detecting any potential health issues early. Your doctor can order a complete blood count (CBC) to assess your ANC and other blood cell counts.
6.6 Consult with Healthcare Professionals
If you have concerns about your ANC levels, it is essential to consult with healthcare professionals for personalized advice and guidance. They can help you identify potential causes of abnormal ANC levels and recommend appropriate management strategies.
7. ANC and Autoimmune Diseases
Autoimmune diseases can significantly impact ANC levels, often leading to neutropenia. In autoimmune disorders, the immune system mistakenly attacks the body’s own tissues, including neutrophils. This can result in a decreased neutrophil count, increasing the risk of infections.
7.1 Mechanisms of Neutropenia in Autoimmune Diseases
Several mechanisms can contribute to neutropenia in autoimmune diseases:
- Antibody-Mediated Destruction: The immune system produces antibodies that target and destroy neutrophils.
- Bone Marrow Suppression: Autoimmune processes can suppress the bone marrow’s ability to produce neutrophils.
- Increased Neutrophil Consumption: Neutrophils may be consumed at a higher rate due to chronic inflammation associated with autoimmune diseases.
7.2 Common Autoimmune Diseases Associated with Neutropenia
Some of the most common autoimmune diseases associated with neutropenia include:
- Systemic Lupus Erythematosus (SLE): SLE is a chronic autoimmune disease that can affect various organs, including the blood cells. Neutropenia is a common complication of SLE.
- Rheumatoid Arthritis (RA): RA is a chronic inflammatory disorder that primarily affects the joints. Neutropenia can occur in some individuals with RA.
- Sjögren’s Syndrome: Sjögren’s syndrome is an autoimmune disease that affects the moisture-producing glands, leading to dry eyes and dry mouth. Neutropenia can occur in some cases.
- Autoimmune Hemolytic Anemia (AIHA): AIHA is a condition in which the immune system attacks and destroys red blood cells. Neutropenia can sometimes occur in association with AIHA.
- Immune Thrombocytopenic Purpura (ITP): ITP is a condition in which the immune system attacks and destroys platelets. Neutropenia can sometimes occur in association with ITP.
7.3 Diagnosis and Management of Neutropenia in Autoimmune Diseases
Diagnosing neutropenia in autoimmune diseases involves assessing ANC levels through a complete blood count (CBC). Further tests may be necessary to determine the underlying cause of neutropenia and to evaluate the activity of the autoimmune disease.
Management of neutropenia in autoimmune diseases typically involves treating the underlying autoimmune condition with medications such as:
- Corticosteroids: Corticosteroids can help suppress the immune system and reduce inflammation.
- Immunosuppressants: Immunosuppressant drugs, such as methotrexate or azathioprine, can help control the autoimmune response.
- Biologic Therapies: Biologic therapies, such as TNF inhibitors or B-cell depleting agents, can target specific components of the immune system.
In some cases, granulocyte colony-stimulating factors (G-CSFs) may be used to stimulate neutrophil production.
7.4 Monitoring and Supportive Care
Individuals with autoimmune diseases and neutropenia require regular monitoring to assess their ANC levels and to detect any signs of infection. Supportive care measures may include:
- Preventive Antibiotics: Antibiotics may be prescribed to prevent bacterial infections.
- Vaccinations: Vaccinations are recommended to protect against preventable infections.
- Hygiene Practices: Good hygiene practices, such as frequent handwashing, are essential to minimize the risk of infection.
8. The Link Between ANC and Viral Infections
Viral infections can have a complex impact on ANC levels. In some cases, viral infections can cause a temporary decrease in ANC, leading to neutropenia. In other cases, viral infections can trigger an increase in ANC, resulting in neutrophilia.
8.1 Mechanisms of ANC Changes in Viral Infections
Several mechanisms can contribute to ANC changes during viral infections:
- Direct Viral Suppression: Some viruses can directly suppress the bone marrow’s ability to produce neutrophils.
- Immune-Mediated Destruction: The immune system’s response to a viral infection can sometimes lead to the destruction of neutrophils.
- Increased Neutrophil Consumption: Neutrophils may be consumed at a higher rate as they fight the viral infection.
- Stimulation of Neutrophil Production: In some cases, viral infections can stimulate the bone marrow to produce more neutrophils.
8.2 Common Viral Infections Associated with Neutropenia
Some of the most common viral infections associated with neutropenia include:
- Influenza (Flu): The flu virus can sometimes cause a temporary decrease in ANC.
- Respiratory Syncytial Virus (RSV): RSV is a common cause of respiratory infections in infants and young children. Neutropenia can occur in some cases.
- Epstein-Barr Virus (EBV): EBV is the virus that causes mononucleosis (mono). Neutropenia can occur during EBV infections.
- Human Immunodeficiency Virus (HIV): HIV can damage the immune system, including the bone marrow, leading to neutropenia.
- Hepatitis Viruses (A, B, C): Hepatitis viruses can sometimes cause neutropenia.
8.3 Management of Neutropenia in Viral Infections
Management of neutropenia in viral infections typically involves:
- Treating the Underlying Viral Infection: Antiviral medications may be prescribed to treat the viral infection.
- Supportive Care: Supportive care measures, such as rest, hydration, and pain relief, can help manage symptoms.
- Monitoring ANC Levels: Regular monitoring of ANC levels is essential to assess the severity of neutropenia.
In severe cases of neutropenia, granulocyte colony-stimulating factors (G-CSFs) may be used to stimulate neutrophil production.
8.4 Prevention of Viral Infections
Preventing viral infections is crucial for maintaining a healthy ANC. Here are some preventive measures:
- Vaccinations: Get vaccinated against preventable viral infections, such as the flu.
- Hand Hygiene: Wash your hands frequently with soap and water.
- Avoid Close Contact with Sick Individuals: Avoid close contact with people who have viral infections.
- Respiratory Etiquette: Cover your mouth and nose when you cough or sneeze.
9. ANC and Benign Ethnic Neutropenia (BEN)
Benign ethnic neutropenia (BEN) is a condition characterized by lower-than-average ANC levels in individuals of certain ethnic backgrounds, particularly those of African, Middle Eastern, and West Indian descent. Despite having lower ANC levels, individuals with BEN typically do not experience an increased risk of infection.
9.1 Prevalence of BEN
BEN is relatively common in certain ethnic groups. It is estimated that 25-50% of individuals of African descent have BEN.
9.2 Genetic Factors in BEN
BEN is thought to be related to genetic variations that affect neutrophil production or function. One of the most well-studied genetic variations associated with BEN is the Duffy-null allele. The Duffy antigen is a protein found on the surface of red blood cells and other cells, including neutrophils. Individuals with the Duffy-null allele do not express the Duffy antigen on their red blood cells. This genetic variation is common in individuals of African descent and is associated with lower ANC levels.
9.3 Clinical Significance of BEN
The primary clinical significance of BEN is that it can be mistaken for other causes of neutropenia, such as chemotherapy-induced neutropenia or neutropenia associated with autoimmune diseases. It is essential to consider the possibility of BEN when evaluating neutropenia in individuals of African, Middle Eastern, or West Indian descent.
9.4 Diagnosis of BEN
BEN is typically diagnosed based on the following criteria:
- Lower-than-average ANC levels in an individual of African, Middle Eastern, or West Indian descent
- Absence of increased risk of infection
- Normal bone marrow examination
9.5 Management of BEN
BEN typically does not require any specific treatment. Individuals with BEN should be educated about the condition and reassured that it is not associated with an increased risk of infection.
9.6 Importance of Awareness
Raising awareness of BEN among healthcare professionals is crucial to avoid unnecessary testing and treatment for individuals with this condition.
10. When to Consult a Doctor About Your ANC
Knowing when to consult a doctor about your ANC is essential for protecting your health. While occasional fluctuations in ANC levels are normal, certain situations warrant medical attention.
10.1 Symptoms of Infection
If you experience symptoms of infection, such as fever, chills, sore throat, cough, or skin infections, it is essential to consult a doctor promptly. These symptoms may indicate that your ANC is low, making you more susceptible to infections.
10.2 Unexplained Neutropenia
If you have an ANC level below the normal range (below 2,500 neutrophils per microliter) without any apparent cause, it is essential to consult a doctor to determine the underlying reason. Unexplained neutropenia may indicate an underlying medical condition that requires treatment.
10.3 Recurrent Infections
If you experience recurrent infections, such as frequent colds, flu, or skin infections, it may be a sign that your ANC is consistently low. In this case, it is essential to consult a doctor to evaluate your immune system and ANC levels.
10.4 Chemotherapy or Radiation Therapy
If you are undergoing chemotherapy or radiation therapy, it is crucial to have your ANC levels monitored regularly by your healthcare team. Chemotherapy and radiation therapy can often cause neutropenia, increasing your risk of infection.
10.5 Autoimmune Diseases
If you have an autoimmune disease, such as lupus or rheumatoid arthritis, it is essential to have your ANC levels monitored regularly, as these conditions can sometimes cause neutropenia.
10.6 Medications
If you are taking medications that can affect ANC levels, such as certain antibiotics or immunosuppressants, it is essential to have your ANC levels monitored regularly.
10.7 Family History of Neutropenia
If you have a family history of neutropenia, you may be at increased risk of developing the condition yourself. In this case, it is essential to talk to your doctor about whether you should have your ANC levels checked.
10.8 Monitoring During Pregnancy
If you are pregnant, it is essential to have your ANC levels monitored as part of your prenatal care. ANC levels can change during pregnancy, and it is essential to ensure that your immune system is functioning properly.
10.9 Proactive Approach
Even if you don’t have any specific symptoms or risk factors, it is always a good idea to talk to your doctor about your ANC levels during your routine checkups. This is particularly important if you have any concerns about your immune system or overall health.
Are you worried about your ANC levels or have questions about your health? Don’t hesitate to seek expert advice. Visit WHAT.EDU.VN today to ask your health-related questions and receive reliable answers from knowledgeable professionals. Your health matters, and we’re here to help you understand and manage it better.
Navigating health concerns can be challenging, but WHAT.EDU.VN is here to simplify the process. Do you have questions about ANC, neutropenia, or any other medical topic? Our platform provides a space to ask questions and receive answers from experts. Join WHAT.EDU.VN today and take control of your health journey. For immediate assistance, contact us at 888 Question City Plaza, Seattle, WA 98101, United States. Whatsapp: +1 (206) 555-7890 or visit our website at what.edu.vn.