What Is The Pathophysiology? Pathophysiology, the functional changes associated with disease or injury, is explained clearly at WHAT.EDU.VN. Discover an easier way to understand disease processes and health conditions. Learn about disease mechanisms, physiological abnormalities, and pathological processes.
1. Understanding Pathophysiology: An In-Depth Exploration
Pathophysiology is the study of how normal body functions are disrupted by disease. It seeks to explain the physiological processes that lead to the signs and symptoms experienced by patients. Understanding pathophysiology is crucial for healthcare professionals to diagnose, treat, and prevent diseases effectively. It bridges the gap between basic sciences like anatomy, physiology, and pathology, providing a functional understanding of disease states.
1.1. Defining Pathophysiology
Pathophysiology, at its core, delves into the functional and physical manifestations of diseases. The term itself is derived from “patho-,” indicating physical changes, and “physio-,” which denotes functional processes. Therefore, pathophysiology encompasses both the observable changes and the underlying mechanisms that occur during a disease process. It explores how diseases alter normal physiological functions, leading to specific signs and symptoms.
1.2. The Importance of Pathophysiology
Understanding pathophysiology is critical for several reasons:
- Diagnosis: It helps healthcare professionals understand the underlying causes of a patient’s symptoms, leading to accurate diagnoses.
- Treatment: It informs the selection of appropriate treatments by targeting the specific mechanisms driving the disease.
- Prevention: Understanding disease processes allows for the development of preventive strategies to reduce the risk of disease development or progression.
- Patient Education: It enables healthcare providers to explain the disease process to patients, promoting adherence to treatment plans and lifestyle modifications.
- Research: It provides a framework for investigating new disease mechanisms and developing novel therapeutic interventions.
1.3. Scope of Pathophysiology
Pathophysiology spans a broad range of topics, including:
- Etiology: The causes or origins of diseases.
- Pathogenesis: The mechanisms by which diseases develop and progress.
- Morphological Changes: The structural alterations in cells, tissues, and organs caused by disease.
- Functional Derangements: The disruptions in normal physiological processes.
- Clinical Manifestations: The signs and symptoms of disease.
1.4. Key Concepts in Pathophysiology
Several key concepts are fundamental to understanding pathophysiology:
- Homeostasis: The body’s ability to maintain a stable internal environment despite external changes. Disease often disrupts homeostasis.
- Cellular Adaptation: Cells can adapt to changes in their environment, but prolonged or severe stress can lead to maladaptation and disease.
- Inflammation: A protective response to injury or infection, but chronic inflammation can contribute to disease.
- Immunity: The body’s defense mechanisms against pathogens, but immune system dysfunction can lead to autoimmune diseases or immunodeficiency.
- Genetic Factors: Genes can predispose individuals to certain diseases.
- Environmental Factors: Exposure to toxins, infections, and other environmental stressors can contribute to disease.
2. Exploring Pathophysiological Mechanisms
Pathophysiology explores various mechanisms by which diseases disrupt normal body functions.
2.1. Genetic Mutations
Genetic mutations can lead to a wide range of diseases by altering protein structure and function. These mutations can be inherited or acquired during an individual’s lifetime.
Examples:
- Cystic Fibrosis: Caused by mutations in the CFTR gene, leading to abnormal chloride transport and thick mucus production in the lungs and other organs.
- Sickle Cell Anemia: Caused by a mutation in the hemoglobin gene, leading to abnormally shaped red blood cells that can block blood flow.
- Huntington’s Disease: Caused by a mutation in the huntingtin gene, leading to progressive neurodegeneration.
2.2. Infectious Agents
Infections caused by bacteria, viruses, fungi, and parasites can disrupt normal body functions and cause disease.
Examples:
- Pneumonia: Infection of the lungs, often caused by bacteria or viruses, leading to inflammation and impaired gas exchange.
- HIV/AIDS: Viral infection that attacks the immune system, leading to immunodeficiency and increased susceptibility to opportunistic infections.
- Malaria: Parasitic infection transmitted by mosquitoes, leading to fever, chills, and anemia.
2.3. Inflammatory Processes
Inflammation is a protective response to injury or infection, but chronic inflammation can contribute to various diseases.
Examples:
- Rheumatoid Arthritis: Autoimmune disease characterized by chronic inflammation of the joints, leading to pain, swelling, and joint damage.
- Inflammatory Bowel Disease (IBD): Chronic inflammation of the digestive tract, including Crohn’s disease and ulcerative colitis, leading to abdominal pain, diarrhea, and bleeding.
- Asthma: Chronic inflammatory disease of the airways, leading to bronchoconstriction, mucus production, and difficulty breathing.
2.4. Metabolic Disorders
Metabolic disorders disrupt normal metabolic processes, leading to imbalances in various substances in the body.
Examples:
- Diabetes Mellitus: Disorder characterized by high blood sugar levels due to defects in insulin production or action.
- Hyperthyroidism: Condition in which the thyroid gland produces too much thyroid hormone, leading to various symptoms such as weight loss, anxiety, and rapid heartbeat.
- Gout: A type of arthritis caused by the buildup of uric acid crystals in the joints, leading to inflammation and pain.
2.5. Degenerative Processes
Degenerative processes involve the progressive deterioration of tissues and organs over time.
Examples:
- Alzheimer’s Disease: Neurodegenerative disease characterized by progressive cognitive decline and memory loss.
- Osteoarthritis: Degenerative joint disease characterized by the breakdown of cartilage, leading to pain, stiffness, and reduced mobility.
- Parkinson’s Disease: Neurodegenerative disease characterized by the loss of dopamine-producing neurons, leading to motor symptoms such as tremors, rigidity, and slow movement.
3. Pathophysiology of Specific Diseases
Understanding the pathophysiology of specific diseases helps healthcare professionals provide targeted and effective treatment. Let’s examine the pathophysiology of several common conditions.
3.1. Cardiovascular Diseases
Cardiovascular diseases are a leading cause of death worldwide. Understanding their pathophysiology is essential for prevention and treatment.
- Atherosclerosis: Characterized by the buildup of plaque in the arteries, leading to reduced blood flow and increased risk of heart attack and stroke. The process begins with damage to the endothelium, the inner lining of the arteries, often caused by factors such as high blood pressure, high cholesterol, smoking, and diabetes. This damage triggers an inflammatory response, leading to the accumulation of lipids, immune cells, and other substances in the artery wall. Over time, these substances form plaque, which can narrow the arteries and restrict blood flow.
- Hypertension: High blood pressure, which can damage blood vessels and increase the risk of heart disease, stroke, and kidney disease. Hypertension can be caused by a variety of factors, including genetics, lifestyle, and underlying medical conditions. The pathophysiology of hypertension involves complex interactions between the heart, blood vessels, kidneys, and nervous system. Increased sympathetic nervous system activity, increased sodium retention by the kidneys, and structural changes in the blood vessels can all contribute to elevated blood pressure.
- Heart Failure: A condition in which the heart is unable to pump enough blood to meet the body’s needs. Heart failure can result from various underlying conditions, such as coronary artery disease, hypertension, and valve disorders. The pathophysiology of heart failure involves a complex interplay of factors, including impaired cardiac contractility, increased afterload, and neurohormonal activation.
3.2. Respiratory Diseases
Respiratory diseases affect the lungs and airways, leading to impaired gas exchange and breathing difficulties.
- Chronic Obstructive Pulmonary Disease (COPD): A progressive lung disease characterized by airflow limitation, often caused by smoking. COPD encompasses two main conditions: emphysema and chronic bronchitis. Emphysema involves the destruction of the alveoli, the tiny air sacs in the lungs, leading to reduced surface area for gas exchange. Chronic bronchitis involves inflammation and narrowing of the airways, leading to increased mucus production and difficulty breathing.
- Asthma: A chronic inflammatory disease of the airways, leading to bronchoconstriction, mucus production, and difficulty breathing. Asthma is characterized by airway hyperresponsiveness, meaning that the airways are overly sensitive to various triggers, such as allergens, irritants, and exercise. Exposure to these triggers leads to inflammation, bronchoconstriction, and mucus production, resulting in symptoms such as wheezing, coughing, and shortness of breath.
- Pneumonia: An infection of the lungs, often caused by bacteria or viruses, leading to inflammation and impaired gas exchange. Pneumonia can be caused by a variety of pathogens, including bacteria, viruses, and fungi. The infection triggers an inflammatory response in the lungs, leading to the accumulation of fluid and immune cells in the alveoli. This impairs gas exchange, resulting in symptoms such as coughing, fever, and shortness of breath.
3.3. Endocrine Disorders
Endocrine disorders involve the dysfunction of endocrine glands, leading to hormonal imbalances and various health problems.
- Diabetes Mellitus: A disorder characterized by high blood sugar levels due to defects in insulin production or action. There are two main types of diabetes: type 1 and type 2. Type 1 diabetes is an autoimmune disease in which the body’s immune system attacks and destroys the insulin-producing cells in the pancreas. Type 2 diabetes is characterized by insulin resistance, meaning that the body’s cells do not respond properly to insulin.
- Hypothyroidism: A condition in which the thyroid gland does not produce enough thyroid hormone, leading to slowed metabolism and various symptoms such as fatigue, weight gain, and depression. Hypothyroidism can be caused by a variety of factors, including autoimmune disease, iodine deficiency, and thyroid surgery. The lack of thyroid hormone leads to slowed metabolism and various symptoms affecting multiple organ systems.
- Hyperthyroidism: A condition in which the thyroid gland produces too much thyroid hormone, leading to accelerated metabolism and various symptoms such as weight loss, anxiety, and rapid heartbeat. Hyperthyroidism can be caused by a variety of factors, including Graves’ disease, thyroid nodules, and excessive iodine intake. The excess thyroid hormone leads to accelerated metabolism and various symptoms affecting multiple organ systems.
3.4. Neurological Disorders
Neurological disorders affect the brain, spinal cord, and nerves, leading to a wide range of symptoms.
- Stroke: Occurs when blood supply to the brain is interrupted, leading to brain cell damage. There are two main types of stroke: ischemic stroke and hemorrhagic stroke. Ischemic stroke is caused by a blockage in a blood vessel supplying the brain, while hemorrhagic stroke is caused by bleeding into the brain. The interruption of blood flow leads to oxygen deprivation and brain cell damage, resulting in various neurological deficits depending on the affected area of the brain.
- Alzheimer’s Disease: A neurodegenerative disease characterized by progressive cognitive decline and memory loss. Alzheimer’s disease is characterized by the accumulation of amyloid plaques and neurofibrillary tangles in the brain. These abnormalities disrupt normal brain function and lead to the progressive loss of cognitive abilities, including memory, language, and executive function.
- Parkinson’s Disease: A neurodegenerative disease characterized by the loss of dopamine-producing neurons, leading to motor symptoms such as tremors, rigidity, and slow movement. Parkinson’s disease is caused by the degeneration of dopamine-producing neurons in the substantia nigra, a region of the brain involved in motor control. The loss of dopamine leads to motor symptoms such as tremors, rigidity, slow movement, and postural instability.
4. Diagnostic Approaches in Pathophysiology
Diagnostic approaches in pathophysiology involve various methods to identify and assess the underlying causes and mechanisms of diseases.
4.1. History and Physical Examination
A thorough history and physical examination are essential first steps in evaluating a patient with suspected disease.
- History Taking: Involves gathering information about the patient’s symptoms, medical history, family history, and lifestyle factors.
- Physical Examination: Involves a systematic evaluation of the patient’s body, including vital signs, inspection, palpation, percussion, and auscultation.
4.2. Laboratory Tests
Laboratory tests provide valuable information about the patient’s physiological state and can help identify abnormalities.
- Blood Tests: Can assess various parameters, such as blood cell counts, electrolytes, glucose levels, liver function, kidney function, and inflammatory markers.
- Urine Tests: Can assess kidney function, detect infections, and identify abnormal substances in the urine.
- Microbiological Tests: Can identify infectious agents, such as bacteria, viruses, and fungi, in various body fluids and tissues.
4.3. Imaging Studies
Imaging studies allow visualization of internal structures and can help identify abnormalities in organs and tissues.
- X-Rays: Use electromagnetic radiation to create images of bones and other dense tissues.
- Computed Tomography (CT) Scans: Use X-rays to create detailed cross-sectional images of the body.
- Magnetic Resonance Imaging (MRI): Uses magnetic fields and radio waves to create detailed images of soft tissues and organs.
- Ultrasound: Uses sound waves to create images of internal structures.
4.4. Genetic Testing
Genetic testing can identify genetic mutations that may be associated with disease risk or diagnosis.
- DNA Sequencing: Determines the order of nucleotides in a DNA molecule.
- Chromosomal Analysis: Examines the structure and number of chromosomes.
- Gene Expression Analysis: Measures the activity of genes in cells and tissues.
4.5. Biopsy
A biopsy involves removing a small sample of tissue for microscopic examination.
- Histopathology: Microscopic examination of tissue samples to identify abnormalities and diagnose diseases.
- Immunohistochemistry: Uses antibodies to detect specific proteins in tissue samples.
5. Therapeutic Interventions Based on Pathophysiology
Understanding the pathophysiology of diseases allows for the development of targeted therapeutic interventions.
5.1. Pharmacological Interventions
Pharmacological interventions involve the use of medications to treat diseases by targeting specific pathophysiological mechanisms.
- Antibiotics: Used to treat bacterial infections by killing or inhibiting the growth of bacteria.
- Antiviral Medications: Used to treat viral infections by inhibiting viral replication.
- Anti-inflammatory Medications: Used to reduce inflammation in various diseases.
- Immunosuppressant Medications: Used to suppress the immune system in autoimmune diseases and organ transplantation.
- Hormone Replacement Therapy: Used to replace deficient hormones in endocrine disorders.
5.2. Surgical Interventions
Surgical interventions involve the use of surgical procedures to treat diseases by correcting anatomical abnormalities or removing diseased tissue.
- Organ Transplantation: Replacement of a diseased organ with a healthy organ from a donor.
- Tumor Resection: Surgical removal of a tumor.
- Angioplasty: A procedure to open blocked arteries in patients with atherosclerosis.
- Valve Replacement: Surgical replacement of a diseased heart valve.
5.3. Lifestyle Modifications
Lifestyle modifications involve changes in diet, exercise, and other lifestyle factors to prevent or manage diseases.
- Dietary Changes: Following a healthy diet can help prevent or manage various diseases, such as diabetes, heart disease, and obesity.
- Regular Exercise: Regular physical activity can improve cardiovascular health, strengthen bones and muscles, and reduce the risk of chronic diseases.
- Smoking Cessation: Quitting smoking can significantly reduce the risk of lung cancer, heart disease, and other smoking-related illnesses.
- Stress Management: Managing stress through techniques such as meditation, yoga, and deep breathing can improve overall health and well-being.
5.4. Gene Therapy
Gene therapy involves the introduction of genes into a patient’s cells to treat or prevent diseases.
- Gene Replacement: Replacing a mutated gene with a normal gene.
- Gene Editing: Correcting a mutated gene using gene editing technologies such as CRISPR-Cas9.
- Gene Augmentation: Introducing a new gene to enhance the function of existing cells.
6. Pathophysiology and Toxicology
In toxicology, pathophysiology examines the biochemical and physical changes that occur when an individual is exposed to harmful amounts of a toxic substance. This includes understanding how the characteristics of the toxicant (such as dosage, physical properties, and chemical properties) interact with the characteristics of the host (including species, life stage, health status, metabolism, and individual sensitivity) to produce physical and/or biochemical changes.
6.1. Host Response to Toxicants
The host’s response to the effects of a toxicant is a crucial aspect of pathophysiology in toxicology. In acute, lethal intoxications, the injury caused by the toxicant may be so severe that it leads to rapid death. In non-lethal exposures, the toxicant-induced injury can result in dysfunction of cells, tissues, or organs, which may persist or progress to death.
6.2. Repair and Adaptation
Persistent toxic injury that does not result in death generally leads to attempts at repair of the toxicant-induced damage. In some cases, the host can develop strategies to adapt to continued exposure to toxicants. These adaptive processes, along with dysfunction and repair, may trigger unregulated cell growth, leading to tumor formation, a process known as carcinogenesis.
6.3. Bioactivation and Detoxification
In many cases, the toxicant itself is the unchanged xenobiotic to which the host was exposed. However, some xenobiotics may be relatively harmless and require bioactivation into more toxic metabolites to exert their effects. The body has endogenous systems to mitigate the effects of many toxicants and their metabolites. When these systems fail, or when the dose of the toxicant exceeds the system’s capacity to neutralize the toxic effects, poisoning occurs, resulting in toxicosis.
6.4. Target Organs and Tissues
Most toxicants exert their effects on specific molecules, tissues, or organs based on their physical and chemical makeup, as well as their absorption, distribution, and metabolism within the body. For example, strong acids or alkalis may cause local injury upon contact with skin, eyes, or mucous membranes without being systemically absorbed. Ingested toxicants are absorbed from the gastrointestinal tract and transported to the liver via the portal vein, where they may cause direct injury, be bioactivated to toxic metabolites, or be detoxified before reaching the general circulation, a process known as the “first pass effect.” Inhaled toxicants, such as smoke, may cause local tissue injury due to irritants or corrosive components, as well as systemic intoxication from toxic gases like carbon monoxide or cyanide.
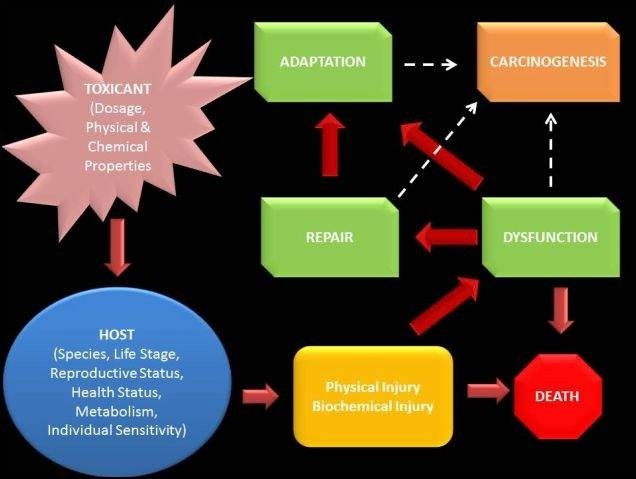 Toxicants Exert Effects
Toxicants Exert Effects
7. Frequently Asked Questions (FAQs) about Pathophysiology
To further enhance your understanding of pathophysiology, here are some frequently asked questions:
| Question | Answer |
|---|---|
| What is the difference between pathology and pathophysiology? | Pathology deals with the study of the causes and nature of diseases, while pathophysiology focuses on the functional changes that occur as a result of these diseases. |
| How does pathophysiology relate to clinical practice? | Understanding pathophysiology is crucial for healthcare professionals to diagnose, treat, and prevent diseases effectively. It helps them understand the underlying mechanisms of disease and select appropriate treatments. |
| Can lifestyle factors influence pathophysiology? | Yes, lifestyle factors such as diet, exercise, smoking, and alcohol consumption can significantly influence pathophysiology by affecting various physiological processes and increasing the risk of certain diseases. |
| What role does genetics play in pathophysiology? | Genetics plays a significant role in pathophysiology, as genetic mutations can predispose individuals to certain diseases or directly cause specific disorders. |
| How does inflammation contribute to pathophysiology? | Inflammation is a protective response to injury or infection, but chronic inflammation can contribute to various diseases, such as rheumatoid arthritis, inflammatory bowel disease, and cardiovascular disease. |
| What are some examples of metabolic disorders in pathophysiology? | Examples of metabolic disorders include diabetes mellitus, hyperthyroidism, and gout, which disrupt normal metabolic processes and lead to imbalances in various substances in the body. |
| How do infectious agents affect pathophysiology? | Infectious agents can disrupt normal body functions and cause disease by directly damaging cells, triggering inflammatory responses, or releasing toxins. |
| What is the importance of diagnostic tests in pathophysiology? | Diagnostic tests, such as blood tests, imaging studies, and biopsies, help identify and assess the underlying causes and mechanisms of diseases, allowing for accurate diagnoses and targeted treatments. |
| How does pathophysiology inform therapeutic interventions? | Understanding the pathophysiology of diseases allows for the development of targeted therapeutic interventions, such as pharmacological interventions, surgical procedures, and lifestyle modifications. |
| What is the role of research in advancing pathophysiology? | Research plays a crucial role in advancing pathophysiology by investigating new disease mechanisms, developing novel therapeutic interventions, and improving our understanding of how diseases affect the body. |
8. Stay Curious and Ask Your Questions at WHAT.EDU.VN
Have more questions about pathophysiology or any other topic? Don’t hesitate to visit WHAT.EDU.VN, where you can ask any question and receive free answers from experts and a knowledgeable community.
We understand the challenges of finding quick, reliable answers to your questions. That’s why we’ve created WHAT.EDU.VN – a platform designed to provide you with the knowledge you need, exactly when you need it.
Why choose WHAT.EDU.VN?
- Free Access: Ask any question, get answers without any cost.
- Fast Responses: Get the answers you need quickly.
- Expert Knowledge: Benefit from the insights of experts.
- Community Support: Engage with a community.
Join us today and experience the ease of having your questions answered at WHAT.EDU.VN.
Address: 888 Question City Plaza, Seattle, WA 98101, United States
WhatsApp: +1 (206) 555-7890
Website: WHAT.EDU.VN
Stop wondering and start learning! Visit what.edu.vn now and ask your question today!